Fentanyl Withdrawal Symptoms and Treatment

Medically Verified: 2/1/24
Medical Reviewer
Chief Editor

All of the information on this page has been reviewed and verified by a certified addiction professional.
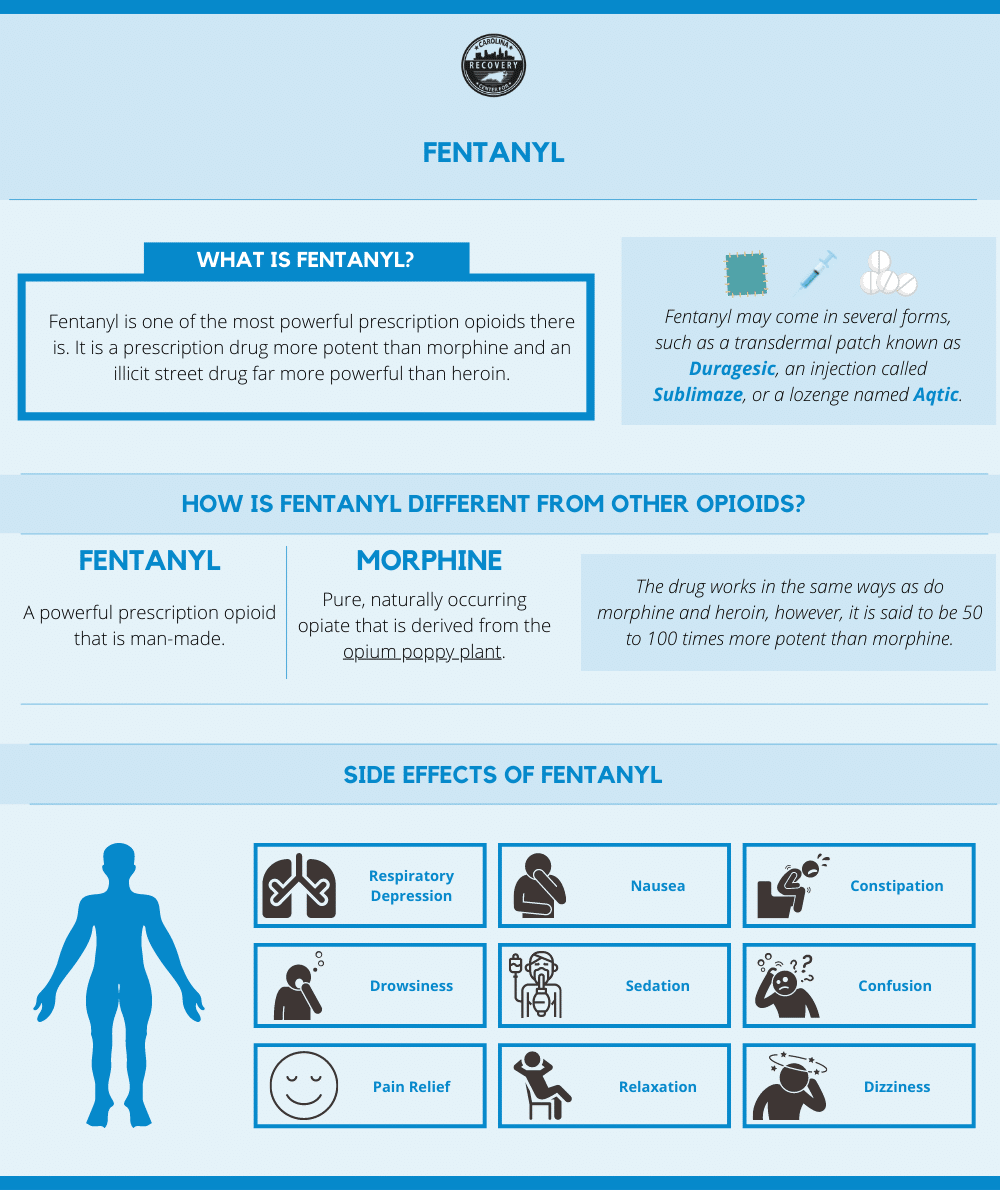
Fentanyl is one of the most powerful prescription opioids there is. It is a prescription drug more potent than morphine and an illicit street drug far more powerful than heroin. Fentanyl may come in several forms, such as a transdermal patch known as Duragesic, an injection called Sublimaze, or a lozenge named Aqtic. The drug works in the same ways as do morphine and heroin, however, it is said to be 50 to 100 times more potent than morphine.[1]
In recent years, fentanyl abuse has risen in the United States and lead to an increasing number of ER visits and opioid-related overdose deaths. While some people abuse fentanyl patches that are prescribed to them, others receive heroin or other drugs that are laced with fentanyl on the streets. Some drug users develop such a high tolerance to heroin that they graduate to using fentanyl. On the other hand, some people, such as cancer patients, require around-the-clock pain management during which they may receive fentanyl. Whatever the case may be, long term use of fentanyl and other opioids will lead to dependence and fentanyl withdrawal when people stop taking the drug.
Long-term opioid abuse of any kind produces changes in the brain so that the brain and body crave opioids and fail to function normally without them. Once physical dependence occurs, withdrawal symptoms set in until the body adjusts and restores balance back to the system. Although fentanyl withdrawal symptoms are typically not deadly, there are serious and should not be taken lightly. Furthermore, people should never stop taking fentanyl “cold turkey.” Instead, it’s best to detox from fentanyl at a medical facility.
Fentanyl Withdrawal Timeline
The duration and severity of opioid withdrawal depend on a number of different factors. These include:
- The dose – people who are used to taking a higher dose will experience symptoms that begin sooner and are more severe than someone who takes a lower dose
- Frequency of use – people who use fentanyl several times throughout the day will experience more severe and longer-lasting symptoms than someone who takes it less frequently
- Co-occurring conditions – people with co-occurring mental or physical health conditions may experience more severe withdrawal
- Method of administration – people who use fentanyl patches may not experience symptoms for up to 24 hours after taking their last dose while someone who injects it will begin experiencing withdrawal symptoms just hours after their last dose.
In general, most users will see their withdrawal symptoms begin within the first 12 hours after their last dose of fentanyl. These symptoms will increase over the first 24 hours and peak between 24-36 hours. Since fentanyl is a fairly fast-acting opioid, most severe withdrawal symptoms subside after 72 hours. After one week, most withdrawal symptoms will subside and people will start feeling better physically.
Fentanyl Withdrawal Symptoms
The symptoms of fentanyl withdrawal are very similar to those of heroin withdrawal. They are often described as flu-like symptoms. These include:[2]
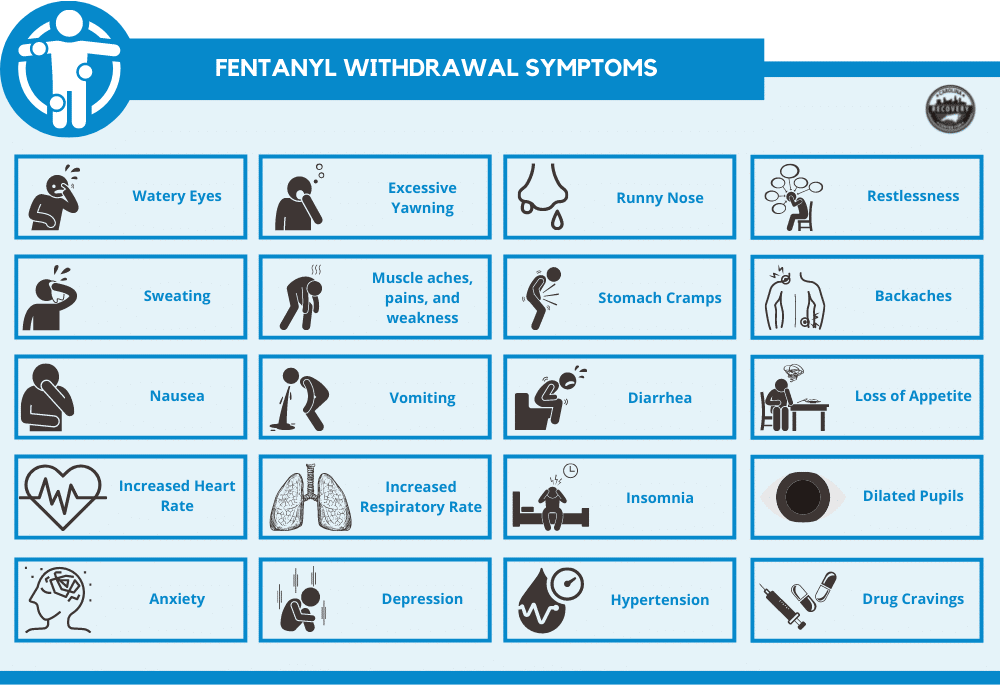
- Overactive tear ducts, watery eyes, and excessive yawning
- Runny nose
- Restlessness
- Sweating
- Chills
- Muscle aches, pains, and weakness
- Stomach cramps
- Backaches
- Nausea and vomiting
- Diarrhea
- Loss of appetite
- Increased heart rate and respiratory rate
- Insomnia
- Dilated pupils
- Anxiety
- Depression
- Hypertension
- Drug cravings
Symptoms such as depression, insomnia, anxiety, and cravings may last longer than a week. Oftentimes, these psychological symptoms are caused by the disruption of dopamine in the brain, making it difficult to feel pleasure. In time and with the help of a comprehensive treatment program, individuals may see these symptoms fade away or learn how to cope with them.
Weaning Off Fentanyl With a Taper
Since stopping fentanyl suddenly can lead to painful withdrawal symptoms, some users may wean themselves off of the drug using a taper. Tapering is usually reserved for people who have been receiving fentanyl for pain management rather than for people who are addicted. A fentanyl taper must always occur under the direction and supervision of a medical professional who can develop a tapering schedule, administer medications, and monitor patients. By slowly removing fentanyl from the system and reducing the dose, withdrawal symptoms can be avoided.
Rather than using fentanyl to taper, patients may be switched to a longer-acting opioid such as methadone or morphine. Once the person switches over to a different opioid, the amount of opioid administered may be reduced by between 20-50% each day until the individual can stop taking opioids completely. Tapering schedules will vary from one person to the next and can last anywhere from five days to two weeks or more.[3]
If you are addicted to fentanyl and are considering trying an at-home taper, you may want to think again. Fentanyl withdrawal is difficult to deal with alone and attempting to manage your own taper may prove impossible. Instead, the best way to detox from fentanyl is to seek help from a medical detox facility.
Medical Detox for Fentanyl Withdrawal Treatment
Detoxification refers to the process of removing drugs and other toxic substances from the body. This process is best performed at a medical detox facility that specializes in substance abuse for the safety and comfort of patients. Detox may be part of an inpatient or outpatient treatment program depending on the severity of the individual’s addiction. Typically, experts recommend that patients detoxing from fentanyl attend a residential detox program so they have access to 24/7 care and support.
Throughout detox, doctors monitor patients’ vital signs and symptoms to ensure their safety. They can administer medications to help reduce symptoms and be prepared to intervene in the event of a medical emergency. Overall, detox usually lasts around one week, but some people will need to stay longer until their symptoms subside completely.
Fentanyl withdrawal is sometimes treated with opioid replacement drugs like buprenorphine. Buprenorphine is a partial opioid agonist that is approved by the FDA to treat opioid dependence and withdrawal. Buprenorphine may come in various forms such as Suboxone, Zubsolv, or Subutex, and the drug binds to opioid receptors in the brain to reduce withdrawal symptoms.[4]
Additional medications like antidepressants, antihistamines, sleep medications, or gastrointestinal medications may also be used to manage additional symptoms. Another medication that is common during fentanyl detox is clonidine – a blood pressure medication that can help regulate increased heart rate, blood pressure, and body temperature.
Find Help for Fentanyl Addiction Today
Fentanyl detox is the safest and most effective way to cope with withdrawal symptoms and get started on the right path toward sobriety. While medical detox is the best way to initially stop fentanyl use and achieve physiological balance, it is equally important to participate in a comprehensive addiction treatment program that uses therapy and medications to help patients stay sober. This way, you can obtain help with drug addiction, mental health, and fentanyl dependence for a full recovery.
If you or someone you know is addicted to fentanyl, you don’t have to endure the withdrawal symptoms on your own. Instead, pick up the phone and contact a dedicated substance abuse treatment provider today to find a drug and alcohol detox and treatment center near you.
References:

