Schizophrenia and Addiction

Medically Verified: 2/1/24
Medical Reviewer
Chief Editor

All of the information on this page has been reviewed and verified by a certified addiction professional.
Schizophrenia is a chronic brain disorder known to affect a person’s ability to think, feel, and behave rationally. The incurable aspect of this mental health condition causes judgment and stigma, however, this disorder is treatable and manageable in many cases. According to research, more than 21 million individuals worldwide are affected by this disease.[1] Unfortunately, research has also found a significant link between schizophrenia, substance abuse, and addiction.
While researchers have found connections between addiction and schizophrenia, there is still plenty of debate on these co-occurring disorders. While some experts feel that individuals with schizophrenia use drugs and alcohol as a means of self-medication, others believe that substance abuse causes the disorder to develop.
Whatever the case may be, it has been proven that substance abuse and schizophrenia co-occur often. Additionally, schizophrenia is known to display similar symptoms as addiction. The similarity in symptoms can make the diagnosis of either disorder difficult, causing individuals to live their lives untreated – without access to recovery.
What is Schizophrenia?
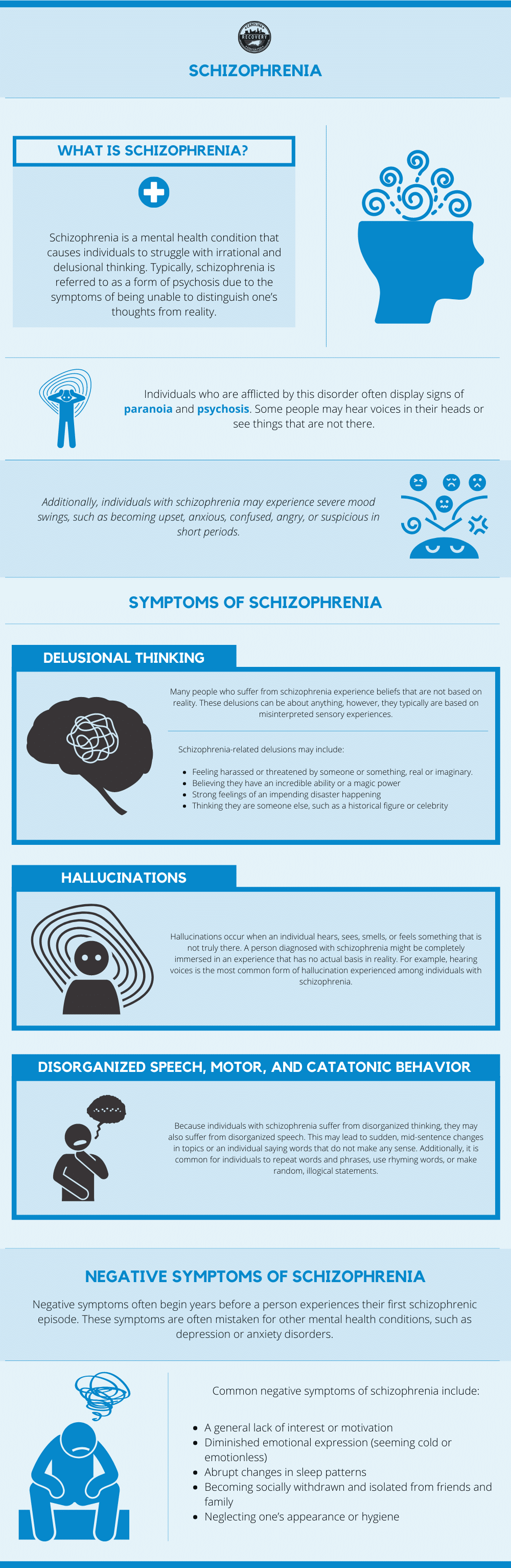
Schizophrenia is a mental health condition that causes individuals to struggle with irrational and delusional thinking. Typically, schizophrenia is referred to as a form of psychosis due to the symptoms of being unable to distinguish one’s thoughts from reality.
Individuals who are afflicted by this disorder often display signs of paranoia and psychosis. Some people may hear voices in their heads or see things that are not there. Additionally, individuals with schizophrenia may experience severe mood swings, such as becoming upset, anxious, confused, angry, or suspicious in short periods. It is important to note that alcohol abuse and mood swings are also connected, proving that schizophrenia and addiction have similarities in symptoms.
Because of the delusional thinking associated with schizophrenia, many individuals do not believe they need help. This may lead to a worsening of symptoms, causing an individual to subconsciously seek forms of self-medication, such as substance abuse and addiction.
The Connection Between Schizophrenia and Addiction
Nearly 50% of individuals with schizophrenia also suffer from addiction and substance abuse issues.[2]
While the abuse of substances does not cause schizophrenia, it can trigger dormant symptoms to appear, acting as an environmental trigger. In other words, an individual with a genetic predisposition for schizophrenia may develop the symptoms after extended periods of substance abuse. Additionally, using substances like marijuana, cocaine, and amphetamines is known to worsen the symptoms of schizophrenia.
Unfortunately, schizophrenia is often difficult to distinguish from addiction due to the similarity in the two disorder’s symptoms. Sometimes, schizophrenia is even mistaken for a substance use disorder because of how similar the symptoms can be. Fortunately, expert researchers continue to study the disorders independently and concurrently to increase the knowledge we have on the co-occurrence of these conditions.
The Symptoms of Schizophrenia
Schizophrenia is known to cause a broad range of symptoms that make it difficult for an individual to function on a normal level. Symptoms may vary and differ in nature, including behavioral, cognitive, and emotional symptoms.
Let’s take a look at the most common symptoms of schizophrenia and how they are linked to addiction.
Delusional Thinking
Many people who suffer from schizophrenia experience beliefs that are not based on reality. These delusions can be about anything, however, they typically are based on misinterpreted sensory experiences.
For example, an individual may believe they are being followed or watched because they saw someone walking behind them. This delusion can continue throughout the day, with the individual believing the same people are coming after them – even though they are only seeing pedestrians walking down the street.
Schizophrenia-related delusions may include:
- Feeling harassed or threatened by someone or something, real or imaginary.
- Believing they have an incredible ability or a magic power
- Strong feelings of an impending disaster happening
- Thinking they are someone else, such as a historical figure or celebrity
It’s important to note that many substances of abuse cause delusional thinking as well. This should not be confused with schizophrenia.
Hallucinations
Hallucinations occur when an individual hears, sees, smells, or feels something that is not truly there. A person diagnosed with schizophrenia might be completely immersed in an experience that has no actual basis in reality. For example, hearing voices is the most common form of hallucination experienced among individuals with schizophrenia.
Once again, this shows a connection between substance use disorders and schizophrenia, as drugs and alcohol may cause individuals to hallucinate when taken frequently or in large doses.
Disorganized Speech, Motor, and Catatonic Behavior
Because individuals with schizophrenia suffer from disorganized thinking, they may also suffer from disorganized speech. This may lead to sudden, mid-sentence changes in topics or an individual saying words that do not make any sense. Additionally, it is common for individuals to repeat words and phrases, use rhyming words, or make random, illogical statements.
This is something that also occurs in individuals with substance abuse issues, for example, in alcoholics. Oftentimes, you hear of alcoholics slurring their words, using words that are made up, or forgetting what they were talking about mid-sentence.
People diagnosed with schizophrenia are known to exhibit disorganized, almost childlike motor behavior. This may include excessive movements, strange postures, and a complete lack of impulse control. Besides, an individual may also go in and out of catatonic states. During a catatonic state, the person will not speak, move or respond to communication.
Negative Symptoms
Schizophrenia includes positive and negative symptoms. Positive symptoms are described as something that schizophrenia has added to an individual’s thinking or behavior. On the other hand, negative symptoms are known as something that schizophrenia has taken away.
Negative symptoms often begin years before a person experiences their first schizophrenic episode. These symptoms are often mistaken for other mental health conditions, such as depression or anxiety disorders.
Common negative symptoms of schizophrenia include:
- A general lack of interest or motivation
- Diminished emotional expression (seeming cold or emotionless)
- Abrupt changes in sleep patterns
- Becoming socially withdrawn and isolated from friends and family
- Neglecting one’s appearance or hygiene
Treatment for Schizophrenia and Addiction
Fortunately, the treatment for schizophrenia and substance use disorder is as similar as the symptoms that both conditions cause. Because of this, treating both disorders simultaneously is possible and effective. Typically, treatment includes a combination of medications, psychotherapy, recovery education, and self-help groups.
If you or a loved one have been diagnosed with co-occurring disorders, Carolina Recovery Center is here to help. With our co-occurring disorders and dual diagnosis treatment track, we are fully equipped to help every patient recover from any combination of mental health conditions that they may struggle with.
Contact us today for a free and confidential consultation.
References:

